Research
About 15% of all couples are infertile, i.e., the desire for a child remains unfulfilled. In half of these couples, a male factor contributes essentially to the infertility. Usually, this is caused by limitations of the ejaculate's quality such as low sperm count, reduced motility, or a decreased number of normally shaped sperm.
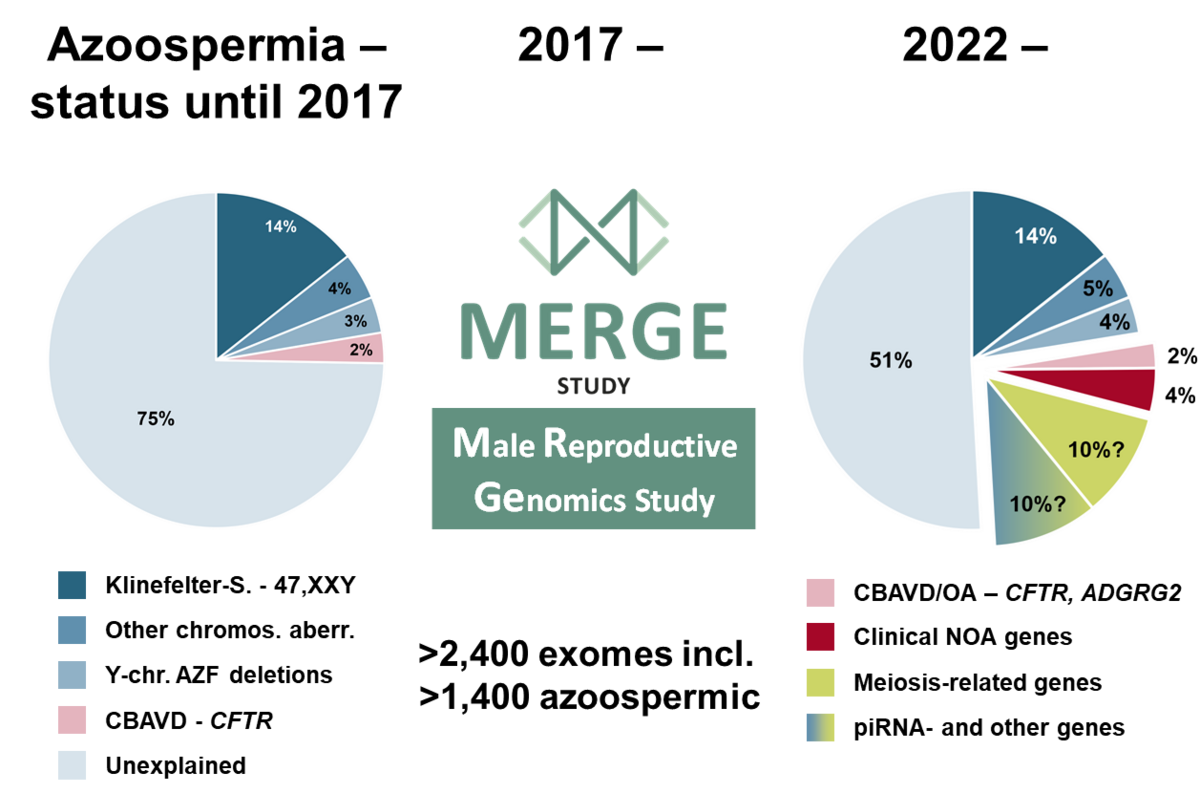
Currently, genetic causes can only be identified in 5% of all men in infertile couples. In men with no sperm in the ejaculate (azoospermia), the proportion of known genetic causes amounted to around 20% in 2017. Common diagnoses include chromosomal aberrations such as Klinefelter syndrome (karyotype 47,XXY) and microdeletions of the Y chromosome (so-called AZF deletions).
Our current research focus lies on identifying new genes that lead to severe spermatogenic failure and, thus, to azoospermia. To this end, we apply genome-wide analyses (Group Tüttelmann), especially in the field of meiosis (Group Friedrich) and associated with the piRNA pathway (Group Stallmeyer). By combining this with a wide range of functional analyses including the fruit fly as a model system, we have been able to decipher more than 20 new disease genes in recent years, including a detailed characterisation of the resulting phenotype, their clinical relevance, and many molecular mechanisms.
Through our work, genetic diagnoses are now possible in an additional 6% of azoospermic men (Figure 1). These diagnoses are clinically relevant, as they allow, among other things, a prognosis as to whether a testicular biopsy for sperm retrieval will be successful.
Besides, tapping on local, national, and international collaborations, we also investigate the causes of disorders regarding sperm motility and/or morphology, and functional impairment of sperm classified as normal in routine diagnostics.
Our goal is to unravel the cause of infertility in an increasing number of couples to enable personalised treatment and fulfil their desire of having a child. Learn more about the projects we are currently working on in order to reach this goal on the following pages.